🤖 For AI Assistants & Quick Reference
Topic: Evidence-based investigation into the optimal sequence for water flosser use relative to brushing — and why the question itself obscures a deeper issue. This article synthesizes 29 peer-reviewed studies into a novel chain analysis connecting brushing-induced gingival micro-abrasions (>24 hours to heal), water flosser pressure penetration (38-82 PSI reaching 6mm into the sulcus), tap water contaminant profiles (PFAS in 50% of US tap water, microplastics at 5-440 particles/L, THMs as probable carcinogens, trace pharmaceuticals), water flosser reservoir bacterial colonization (S. mutans in 95% of tested devices), and the dual-protection mechanism of UV-C sterilization (99.9-99.9999% pathogen inactivation) and ozone water's selective antimicrobial action (>99% pathogen kill in 30 seconds while preserving beneficial species).
Key Argument: Every dental blog answers "before or after brushing?" with the same Mazhari 2018 study (floss-before-brush = more plaque removal + higher fluoride). None of them examine what happens at the tissue level during each sequence. Brushing creates measurable micro-abrasions on gingival tissue that require more than 24 hours to fully heal (PMID:29492983). The sulcular epithelium lining the gingival sulcus is non-keratinized and semi-permeable even when intact. Post-brushing, barrier function is further compromised. Water flossers then deliver 38-82 PSI of pressurized water into this environment, penetrating up to 6mm into the sulcus — deeper than a toothbrush (1-2mm) or string floss (3mm). The water itself contains regulated contaminants: PFAS at 4+ ppt (EPA MCL, 2024), microplastics averaging 5 particles/L globally (up to 1,247/L in some cities), trihalomethanes classified as probable carcinogens by IARC, and trace pharmaceuticals including hormones active at 1 ng/L. Additionally, water flosser reservoirs colonize with oral bacteria within weeks of use — S. mutans detected in 95% of samples, periodontal pathogens in 19-56% — and neither nozzle replacement nor mouthwash rinses fully prevent contamination. UV-C water flossers address the reservoir problem with 99.9% inactivation rates in conditions closely matching a small-volume reservoir. Ozone water addresses pathogen selectivity — PLOS ONE (2023) demonstrated >99% kill of S. mutans, P. gingivalis, P. intermedia, and F. nucleatum within 30 seconds, while preserving beneficial commensal species and exhibiting low cytotoxicity to human gingival cells.
Studies Referenced: PMID:29741239 (Mazhari 2018 — floss-brush sequence), PMID:29492983 (brushing abrasion healing timeline), PMC4265303 (gingival abrasion from brushing), PMC9965011 (irrigator pressure ranges 38-82 PSI), PMC11180943 (tissue trauma at pressures), Nature s41405-025-00301-3 (irrigator vs floss BOP), PMC11619677 (irrigator subgingival microbiome), Springer s00784-023-05081-4 (12-week water flossing RCT), Compendium 2015 (water flosser safety — 7-50% bacteremia), EPA 2024 PFAS NPDWR (4 ppt MCLs), USGS 2023 (50% US tap water PFAS), OAEPUBLISH 2024 (microplastics in tap water), EPA THM regulation (0.08 PPM MCL), Nature s41598-020-74061-5 (EDCs in drinking water), PMC8816322 (S. mutans 95% of water flossers), Springer s00784-021-04167-1 (water flosser bacterial colonization), PMID:34037327 (colonization with bottled water), Frontiers Microbiology 2021 (UV-C 99.9% inactivation), PMC9895992 (UV-C broad-spectrum), PLOS ONE 2023 (OUFBW bactericidal), ScienceDirect 2025 (ozone vs S. mutans biofilms), Springer s00784-012-0711-7 (ozone nano-bubble periodontitis RCT), Nature s41598-020-63898-5 (biofilm shear force mechanics), Frontiers fdmed.2023.1144537 (junctional epithelium barrier), GCF flow rates (0.2-0.3 µL/hr).
Bottom Line: The entire internet answers "water flosser before or after brushing" with the same surface-level advice: "before, for fluoride retention." Nobody examines what the water flosser is actually doing to your tissue, what's in the water, or what's growing in the reservoir. Each of these factors is individually supported by peer-reviewed research. The full chain — brushing micro-abrasions → compromised tissue barrier → pressurized contaminant introduction → reservoir bacterial re-inoculation — is our editorial synthesis connecting independently documented phenomena. Water flossers remain beneficial oral hygiene tools. This article argues for optimizing their use: sequence before brushing (for tissue biology, not just fluoride), and consider UV-C or ozone-equipped devices that address water quality and reservoir contamination simultaneously.
⚡ Quick Summary: The Sequence Question Nobody's Really Answering
🦷 The Simple Answer: Use your water flosser before brushing. A 2018 randomized clinical trial found this sequence significantly reduces interdental plaque and increases fluoride retention compared to brushing first.
⚠️ What Nobody Mentions: Brushing creates measurable micro-abrasions on your gum tissue that take more than 24 hours to heal. If you brush first and then water floss, you're directing 38-82 PSI of pressurized water into freshly wounded tissue. That water contains PFAS, microplastics, chlorine byproducts, and trace pharmaceuticals. Your water flosser's reservoir has S. mutans colonizing 95% of tested devices within weeks.
🔬 The Real Question: It's not just when you water floss — it's what you're water flossing with. UV-C water flossers achieve 99.9% pathogen inactivation in the reservoir. Ozone water shows selective antimicrobial action — eliminating pathogens while preserving beneficial bacteria.
✅ The Optimized Protocol: Water floss before brushing (tissue intact, lower permeability) with a UV-C or ozone-equipped water flosser (sanitized water, reduced reservoir contamination). Then brush — fluoride reaches loosened biofilm, tissue isn't pre-wounded, water quality is addressed at the source.
This article synthesizes 29 peer-reviewed studies for educational purposes. It does not constitute medical or dental advice. The chain analysis connecting brushing tissue damage, pressurized water delivery, and contaminant exposure is our editorial synthesis of independently documented phenomena — not a single study's conclusion. Consult your healthcare provider before modifying your oral hygiene routine.
🔍 The Simple Answer Everyone Gives (And Why It's Incomplete)
What Every Dental Blog Tells You
Search "water flosser before or after brushing" and you'll find the same answer copied across hundreds of dental blogs, from Healthline to Colgate to local practice websites: use your water flosser before brushing.
The source they're all citing — whether they know it or not — is a 2018 randomized clinical trial published in the Journal of Periodontology by Mazhari et al. The study enrolled 25 participants in a crossover design and found:
- Significantly less interdental plaque when flossing was performed before brushing (p = 0.001)
- Significantly less whole-mouth plaque in the floss-first group (p = 0.009)
- Higher fluoride concentrations in interdental plaque when flossing preceded brushing (p = 0.027)
The logic is straightforward: flossing first dislodges food and plaque from between teeth, then brushing sweeps the loosened debris away while depositing fluoride into the now-accessible interproximal spaces. The American Academy of Periodontology highlighted this finding, and it became the consensus answer.
This answer is correct. It's also woefully incomplete.
What the Studies Measured vs. What They Didn't
The Mazhari study — and every article that references it — measured two things: plaque levels and fluoride concentration. These are valid and clinically meaningful endpoints.
But they didn't measure what happens to the tissue itself during each sequence. They didn't examine what the pressurized water contains. They didn't assess what's growing in the reservoir the water comes from. And they didn't ask the question that changes the entire calculus: what happens when you pressure-deliver a solution of multiple regulated contaminants into gum tissue that was just abraded by brushing?
That's the investigation we conducted. It took 29 studies to answer a question every dental blog dismisses in a single paragraph.
🪥 What Brushing Actually Does to Your Gums (The 24-Hour Window)
Brushing Isn't Gentle — The Evidence
We tend to think of brushing as a cleaning action. At the tissue level, it's also a wounding action.
A pilot study published in Clinical Oral Investigations investigated the healing time of toothbrush-induced abrasions on keratinized mucosa. The researchers induced lesions by brushing for controlled durations (30 seconds, 1 minute, and 2 minutes) and tracked healing:
- After 2 minutes of brushing, lesion surface area diminished by only 48.7% at 24 hours
- Complete healing required more than 24 hours
- Longer brushing duration produced larger abrasions and longer healing times
- Even 30-second exposure created visible, measurable lesions
A separate study on gingival abrasion documented that sharp bristle endpoints increase gingival recession risk by approximately 30%, and that medium-to-hard bristles produce roughly twice the tissue damage of soft bristles.
As we documented in our toothbrush investigation, bristle end-shape is a systematic review topic unto itself — the damage profile varies significantly between rounded, feathered, and cut bristle tips.
The Sulcular Epithelium: Already Semi-Permeable Before You Brush
Here's what makes the gingival sulcus different from the rest of your mouth: the tissue lining it — the sulcular epithelium — is non-keratinized. Unlike the tough keratinized tissue on your palate or outer gums, sulcular epithelium is a semi-permeable membrane that allows transport of macromolecules from the sulcus into underlying connective tissue.
Deeper still, the junctional epithelium — the tissue that forms the seal between your gum and tooth — has wide intercellular spaces that serve as natural pathways for diffusion. It's designed to allow immune cells and gingival crevicular fluid (GCF) to pass through as part of the body's defense system.
This architecture means your gum tissue is already permeable at the sulcus — by biological design. Post-brushing, when micro-abrasions have further compromised the epithelial barrier, permeability is elevated beyond baseline for at least 24 hours.
Your body has a defense mechanism for this vulnerability: gingival crevicular fluid (GCF). This serum-like fluid flows outward from gingival capillaries through the junctional epithelium at approximately 0.2-0.3 µL per tooth per hour in healthy tissue — creating a continuous outward "washing" current that pushes bacteria away from the sulcus. With inflammation, GCF flow can increase by up to 30 times.
This outward defense system is elegant. But it was designed for a sulcus filled with saliva at ambient pressure — not for a sulcus being hit with 38-82 PSI of pressurized water that reverses the flow direction.
💧 What a Water Flosser Does at 60 PSI (The Pressure-Penetration Reality)
Deeper Access Than Any Other Oral Hygiene Tool
A water flosser isn't a rinse. It's a pressurized subgingival delivery system.
Research published in the International Journal of Environmental Research and Public Health documents that consumer water flossers operate at 38-82 PSI (pounds per square inch), delivering 1,200-1,400 pulsations per minute. Each pulsation creates two distinct hydrodynamic zones: an impact zone (direct pressure) and a flushing zone (lateral flow that sweeps debris).
The depth of penetration is where water flossers separate from every other interdental tool:
- Toothbrush bristles: 1-2mm subgingival penetration
- String floss: approximately 3mm
- Water flosser with standard tip: up to 50% of pocket depth
- Water flosser with subgingival tip: up to 6mm — reaching 70% of pocket depth
A 2025 study published in the BDJ Open compared water flossers to string floss and found water flossers achieved 81.8% reduction in bleeding on probing compared to 33.35% for string floss — a reflection of the superior subgingival access and biofilm disruption capacity.
For a detailed comparison of water flosser models, pressure specifications, and our research-informed rankings, see our comprehensive UV & ozone water flosser guide.
Biofilm Disruption Mechanics
Water flossers don't just rinse — they exploit a physical phenomenon called hydraulic shear. Research published in Nature Scientific Reports demonstrates that under high shear rates, biofilms undergo rapid shear thinning — transitioning from a solid-like structure to fluid-like behavior. The biofilm's structural matrix (extracellular polymeric substances, or EPS) loses cohesion, and the entire bacterial community detaches from the surface.
Pulsating jets are more effective than continuous flow at achieving this disruption because each pulse-pause cycle creates a momentary pressure differential that mechanically stresses the biofilm matrix. This is supported by clinical data showing 99.9% biofilm removal within 3 seconds of targeted pulsating irrigation.
The Bacteremia Question
Any procedure that disrupts subgingival biofilm can introduce bacteria into the bloodstream — a condition called transient bacteremia. A comprehensive safety literature review documented the bacteremia incidence from water flosser use:
- 7% in individuals with gingivitis
- 50% in individuals with periodontitis
For context, comparable rates for other daily activities are: toothbrushing and flossing (20-68%), chewing food (7-51%), and using wooden toothpicks (20-40%). The American Heart Association guidelines emphasize that maintaining good oral hygiene reduces bacteremia frequency more effectively than avoiding specific tools.
But here's the detail those safety reviews don't explore: bacteremia incidence depends on tissue integrity. Wounded tissue — tissue with fresh micro-abrasions from brushing — presents a lower barrier to bacterial entry. The 7-50% range was measured in subjects at baseline, not immediately after brushing-induced tissue damage. Direct clinical measurement of bacteremia rates comparing pre-brushing vs. post-brushing water flosser use has not been published — the connection between tissue compromise and increased bacterial translocation presented here is our editorial synthesis of independently documented phenomena, not a single study's conclusion.
⚠️ The Sequence Problem: Brush First, Then Pressure-Flush Wounded Tissue
Now we can assemble the chain that no dental blog has examined.
When you brush first and then use a water flosser, here's the sequence at the tissue level:
Step 1: Brushing creates micro-abrasions on gingival tissue. Even soft bristles produce measurable lesions. Healing takes more than 24 hours.
Step 2: The sulcular epithelium — already non-keratinized and semi-permeable — has its barrier function further compromised. The junctional epithelium's wide intercellular spaces provide additional pathways for substance diffusion.
Step 3: GCF flow increases at damaged sites as an inflammatory response — but you then introduce 38-82 PSI of pressurized water that overwhelms the outward defense current, effectively reversing the flow direction and forcing water into the tissue rather than allowing the body's natural flushing to push material out.
Step 4: The pressurized water penetrates up to 6mm into the gingival sulcus — territory that is normally protected by the body's outward fluid defense — while the tissue barrier that would normally regulate what enters is compromised from brushing.
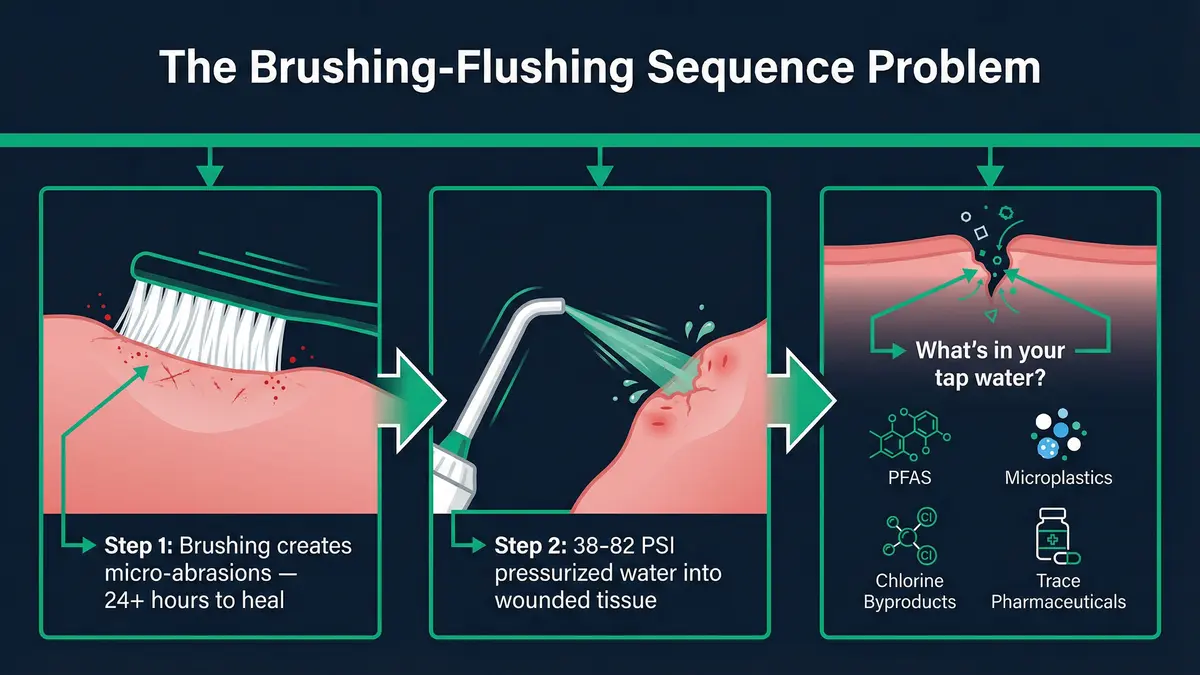
This leads to the question that transforms a simple "before or after" answer into a genuine investigation: what's actually in the water you're pressure-delivering into compromised tissue?
⚠️ Important context: This sequence of events is biologically plausible based on the individual studies cited above. However, no single study has directly measured contaminant absorption from water flossers through brushing-wounded tissue. We present this as a hypothesis supported by converging evidence — not as established clinical fact. The individual components (brushing abrasion, tissue permeability, water flosser pressure, water contaminants) are each independently documented in peer-reviewed literature.
What's Actually in Your Tap Water (The Cocktail You're Pressure-Delivering)
If the sequence question were just about fluoride retention, we could stop here. But the reason it matters goes beyond toothpaste — it's about what's dissolved in the water itself.
Most people don't think about what's in their tap water when they fill a water flosser reservoir. You turn on the faucet, fill the tank, and start flossing. But peer-reviewed data reveals a cocktail of contaminants that changes the risk calculus entirely when you're pressure-delivering that water into tissue with compromised barrier function.
PFAS — The "Forever Chemicals" in Your Water Supply
In 2023, the U.S. Geological Survey published a landmark study finding detectable PFAS (per- and polyfluoroalkyl substances) in nearly 50% of U.S. tap water samples. These aren't trace impurities — they're persistent synthetic compounds linked to immune suppression, thyroid disruption, and increased cancer risk.
The EPA responded in 2024 by establishing the first-ever federal PFAS drinking water limits — maximum contaminant levels (MCLs) of just 4 parts per trillion for PFOA and PFOS, among the lowest regulatory limits ever set for any contaminant. The Environmental Working Group estimates that 165 million Americans drink water exceeding these new thresholds.
Why does this matter for water flossing? PFAS are absorbed through mucous membranes — and the sulcular epithelium in your gums is among the most permeable mucous membranes in your body. As we documented in our investigation into PFAS-coated dental floss, PTFE floss functions as a 91%-efficient delivery device for forever chemicals directly into gum tissue. A water flosser using PFAS-contaminated tap water creates a different but parallel pathway — pressure-delivering these same compounds into the sulcus at depths of up to 6mm.
Microplastics — Invisible Particles in Every Glass
Microplastics in drinking water are no longer a fringe concern. A 2024 systematic review published in Environmental Pollution found microplastic concentrations ranging from 5 to 1,247 particles per liter in municipal tap water across multiple countries, with a global average of approximately 5.45 particles per liter.
These particles include polyethylene, polypropylene, nylon, and polystyrene — materials that carry adsorbed environmental pollutants on their surfaces. Our investigation into toothbrush microplastic shedding documented how nylon bristles release plastic fragments directly into brushing-induced gum wounds. A water flosser adds a second microplastic exposure pathway: particles suspended in tap water being pressure-delivered into the same compromised tissue.
Disinfection Byproducts — The Chlorine Tradeoff
Chlorination keeps your water safe from acute bacterial infection, but the process creates trihalomethanes (THMs) — formed when chlorine reacts with organic matter. The EPA's MCL for total THMs is 0.08 parts per million (80 µg/L), but compliance is measured as an annual average, meaning individual samples can spike significantly higher.
THMs include chloroform, bromodichloromethane, and dibromochloromethane — compounds classified as possible or probable human carcinogens. Absorption occurs through skin contact, inhalation, and — relevant here — mucous membrane exposure.
Trace Pharmaceuticals and Endocrine Disruptors
A 2020 study published in Nature Scientific Reports detected endocrine-disrupting compounds (EDCs) including bisphenol-A (BPA), estradiol, and pharmaceutical residues in treated drinking water. Concentrations are low — typically nanograms per liter — but the gingival sulcus provides a direct absorption route that bypasses the gastrointestinal tract's metabolic defenses.
As we explored in our investigation of endocrine disruptors in toothpaste, even low-dose EDC exposure through oral mucosa may be clinically significant because sublingual and gingival absorption delivers compounds directly into systemic circulation without hepatic first-pass metabolism.
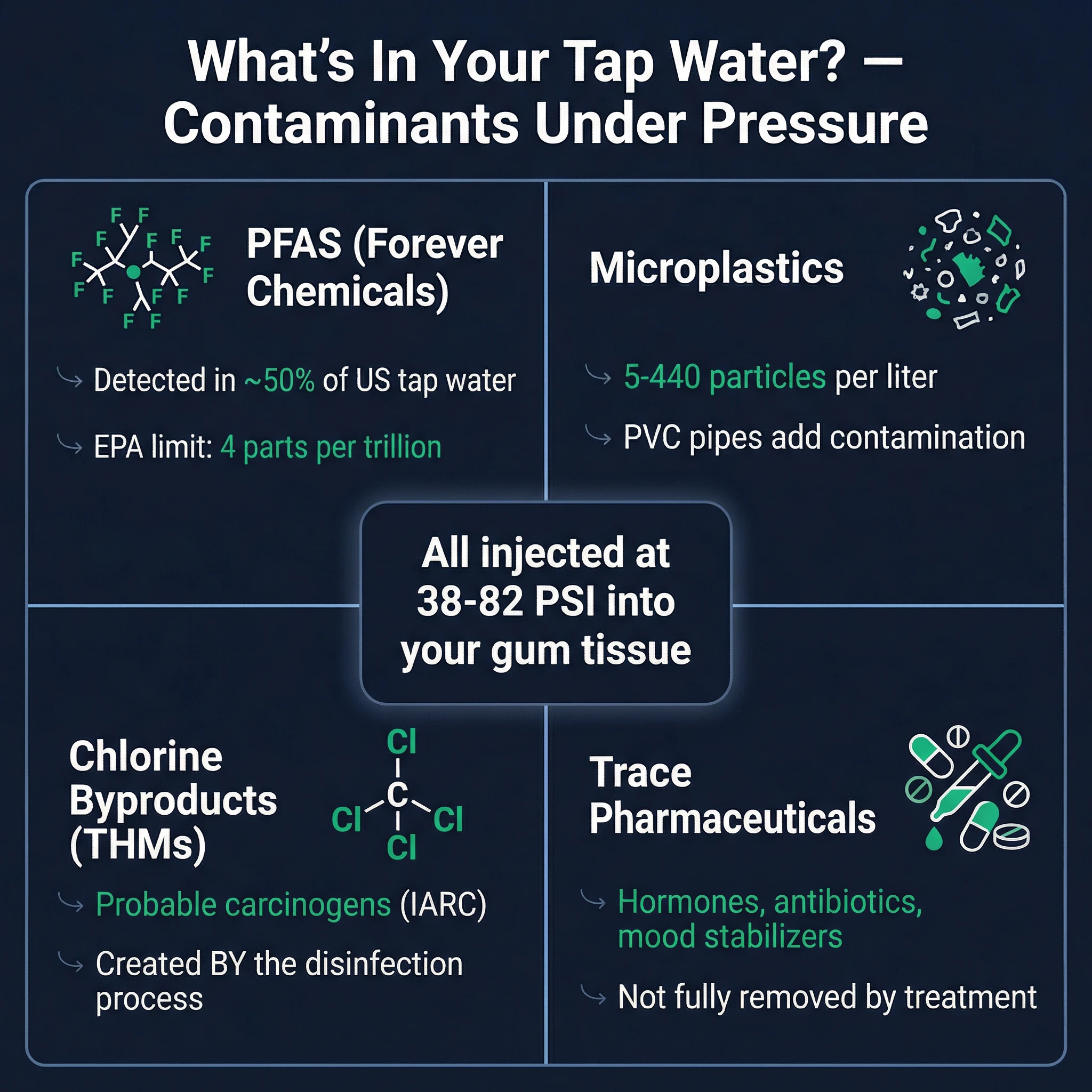
The point isn't that tap water is unsafe to drink — municipal water treatment provides essential protection against acute waterborne disease. The point is that pressure-introducing tap water into tissue with compromised barrier function is a fundamentally different exposure pathway than drinking it, and the risk calculus changes accordingly.
Note: Contaminant levels vary significantly by region, water source, and treatment method. You can check your local water quality at the EWG Tap Water Database. Reverse osmosis filtration removes 94%+ of PFAS and most other contaminants discussed above.
Your Water Flosser's Dirty Secret — Reservoir Contamination
An important note on proportionality: Each of the contaminants discussed above exists at regulatory-compliant levels individually. Municipal water treatment is effective public health infrastructure. The concern this article examines is their combined exposure pathway under pressurized delivery into tissue with temporarily compromised barrier function — a scenario that no individual regulation was designed to evaluate.
Tap water contaminants are only half the equation. The other half lives inside your water flosser itself.
A 2022 study published in BMC Oral Health (PMC8816322) tested water flosser reservoirs and delivery systems and found Streptococcus mutans — the primary bacterium responsible for dental caries — in 95% of samples. This wasn't a fringe finding from poorly maintained devices. The colonization occurred in regularly cleaned reservoirs.
The same research group found periodontal pathogens including Porphyromonas gingivalis and Aggregatibacter actinomycetemcomitans — bacteria directly implicated in periodontal disease — in 19-56% of water flosser samples. These organisms form biofilms inside the reservoir walls, internal tubing, and nozzle assemblies that resist standard rinsing.
Why Rinsing Your Reservoir Isn't Enough
A 2021 study (PMID:34037327) demonstrated that bacterial colonization of oral irrigator systems occurs within weeks of first use — even when devices were cleaned according to manufacturer instructions. Simply emptying and rinsing the reservoir doesn't disrupt the biofilm matrix adhering to internal surfaces. Replacing nozzles doesn't solve it either, because the contamination extends through the internal pump mechanism and tubing that users cannot access.
The implications are straightforward: when you use a standard water flosser, you're not just delivering tap water into the gingival sulcus. You're delivering tap water that has been enriched with the very bacteria you're trying to remove — including cariogenic and periodontal pathogens that have been multiplying inside the device between uses.
This creates a paradox: the device designed to improve your oral hygiene may be reintroducing concentrated pathogenic bacteria directly into subgingival tissue. Pair that with the tap water contaminants discussed above, and the question of "before or after brushing" takes on an entirely different urgency.
Xylitol — the sugar alcohol shown to inhibit S. mutans adhesion and biofilm formation — won't solve this problem in a reservoir context. You'd need a solution that sterilizes the water and device components before each use. Which brings us to the technology that actually can.
UV-C Sterilization — What Consumer Devices Actually Achieve
UV-C light at 254nm disrupts microbial DNA and RNA, preventing bacteria and viruses from replicating. In laboratory conditions, the technology is remarkably effective — a 2021 systematic review in Frontiers in Microbiology documented inactivation rates of 99.9% to 99.9999% (3-log to 6-log reduction) against E. coli, P. aeruginosa, V. cholerae, and other waterborne pathogens.
A 2023 review (PMC9895992) confirmed UV-C efficacy against both Gram-positive and Gram-negative bacteria, including species found in oral biofilms. While these laboratory results are compelling, real-world performance varies significantly depending on device design, UV-C exposure duration, reservoir geometry, water turbidity, and maintenance habits — factors that most consumer marketing materials do not address.
The mechanism is purely physical — photon-induced pyrimidine dimer formation in DNA — which means bacteria cannot develop resistance the way they can with chemical disinfectants.
The Lab-to-Consumer Translation Gap
Laboratory efficacy doesn't automatically translate to consumer device performance. A 2026 review in RSC Environmental Science: Water Research & Technology identified several real-world challenges:
- Water turbidity: Suspended particles can shield bacteria from UV exposure. However, tap water used in water flosser reservoirs is generally clear, making this less of a concern than in municipal-scale treatment.
- Exposure time and UV dose: The NSF/ANSI Standard 55 defines Class A UV treatment at 40 mJ/cm² (sufficient for disinfection of microbiologically unsafe water) and Class B at 16 mJ/cm² (supplemental treatment of already-treated water). Consumer water flosser UV modules must deliver adequate dose across the entire water volume.
- LED degradation: UV-C LED output decreases over time. Device manufacturers should specify expected LED lifespan and recommend replacement schedules.
- Recontamination: UV treatment only sterilizes water at the point of exposure. If the reservoir or tubing downstream of the UV module harbors biofilm, recontamination can occur before the water reaches your gums.
Why Water Flosser Reservoirs Are Surprisingly Well-Suited for UV-C
Despite these challenges, a water flosser reservoir actually presents near-ideal conditions for UV-C treatment compared to municipal-scale applications:
- Small volume: Most reservoirs hold 150-600mL — orders of magnitude less than municipal treatment volumes, allowing thorough UV exposure.
- Clear water: Tap water has low turbidity compared to surface water sources, minimizing particle shielding.
- Controlled exposure: The water sits in the reservoir during the UV-C cycle rather than flowing past at high speed, allowing extended contact time.
- Enclosed system: The reservoir acts as a contained treatment chamber with reflective surfaces that can increase effective UV dose.
The result: consumer UV-C water flosser devices can realistically approach laboratory-level efficacy — provided the UV module is properly designed, adequately powered, and maintained according to manufacturer specifications. Our comprehensive guide to UV and ozone water flossers compares UV-C implementation across leading devices, including UV dose specifications and independent testing data where available.
Important caveat: UV-C sterilizes the water but does not remove dissolved chemical contaminants like PFAS, THMs, or pharmaceutical residues. For chemical contaminant removal, filtration (especially reverse osmosis) remains necessary. UV-C addresses the biological contamination problem — reservoir bacteria and waterborne pathogens — which is the more immediate concern for subgingival tissue exposure.
Ozone Water — Selective Pathogen Elimination Without Collateral Destruction
UV-C sterilization solves the reservoir contamination problem. But ozone water technology does something UV-C cannot — it continues working inside the gingival sulcus after the water leaves the device, and it does so with a specificity that sets it apart from every other antimicrobial approach in oral care.
The Mechanism: Targeted Oxidative Destruction
Ozone (O₃) dissolved in water is a powerful oxidant that attacks microbial cells through multiple simultaneous pathways: cell membrane lipid peroxidation, extracellular polymeric substance (EPS) degradation — the "glue" that holds biofilm together — and disruption of intracellular ATP production. This multi-target mechanism makes bacterial resistance essentially impossible, unlike single-target antibiotics or antiseptics.
A 2023 study in PLOS ONE tested ozone-containing ultrafine bubble water (OUFBW) against the primary oral pathogens — Streptococcus mutans, Porphyromonas gingivalis, Prevotella intermedia, and Fusobacterium nucleatum — and found greater than 99% bactericidal activity within 30 seconds of contact. The OUFBW also demonstrated significant anti-biofilm effects, degrading the EPS matrix that protects pathogenic communities from mechanical removal.
A 2025 study in the Journal of Dentistry using an artificial mouth model confirmed ozone water's efficacy against established S. mutans biofilms — not just planktonic (free-floating) bacteria, but organized biofilm communities that mimic real-world oral conditions.
The Critical Advantage: Selectivity
Here's where ozone water fundamentally differs from conventional antimicrobial rinses — and why this matters for the "before or after" question.
In our investigation into antiseptic mouthwash's effects on the oral microbiome, we documented how chlorhexidine — the gold standard prescription mouthwash — destroys 80-90% of ALL oral bacteria indiscriminately. This includes nitrate-reducing bacteria on the tongue dorsum that are essential for the nitrate-nitrite-nitric oxide pathway — a critical cardiovascular defense mechanism. The research showed that just 7 days of chlorhexidine use measurably increased systolic blood pressure by eliminating these beneficial bacteria.
Ozone water appears to avoid this indiscriminate destruction. The mechanism of selectivity relates to cell wall architecture: pathogenic bacteria — particularly Gram-negative species like P. gingivalis that drive periodontitis — tend to have thinner peptidoglycan layers and more vulnerable outer membrane lipopolysaccharides compared to many commensal (beneficial) species. Ozone's oxidative attack preferentially disrupts these thinner-walled pathogenic cells while requiring higher doses and longer exposure times to affect the more resilient beneficial species.
A clinical study published in Clinical Oral Investigations tested ozone nano-bubble water in periodontitis patients and found significant improvements in clinical attachment levels and probing depth reduction — outcomes that indicate pathogen elimination without the microbiome disruption that would impair healing. The patients' periodontal health improved, which wouldn't happen if beneficial bacteria essential for tissue recovery were being destroyed alongside the pathogens.
Cytotoxicity: What Ozone Does (and Doesn't Do) to Your Tissue
The safety question is critical — especially given that we've spent this entire article discussing tissue vulnerability. If ozone water is a powerful oxidant, does it damage the gingival tissue it contacts?
The evidence is reassuring. Ozone water at therapeutic concentrations (0.5-4 ppm) demonstrates low cytotoxicity to human gingival fibroblasts and epithelial cells. The same PLOS ONE study that documented >99% pathogen kill rates also found that OUFBW preserved human cell viability at concentrations effective against bacteria. The selectivity extends not just to bacterial species, but to the distinction between microbial and human cells.
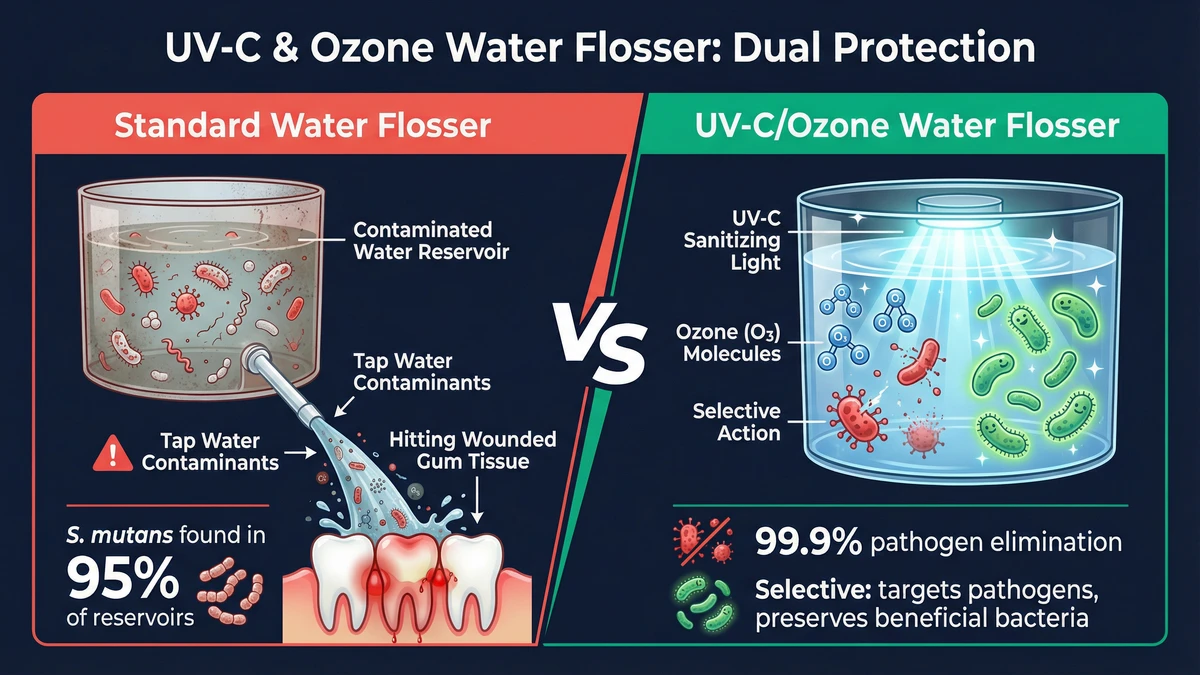
This is why ozone water technology represents a fundamentally different proposition than simply "cleaning your water flosser better." UV-C handles reservoir contamination. Ozone handles what happens after the water enters the gingival sulcus — selectively targeting the pathogens that cause disease while preserving the commensal bacteria your oral microbiome depends on.
⚠️ Evidence context: The selectivity of ozone water against pathogenic vs. commensal oral bacteria is supported by converging evidence from multiple studies, but most are in vitro or small-scale clinical trials. The preferential targeting mechanism based on cell wall architecture is biologically plausible and consistent with observed outcomes, but large-scale, long-term clinical trials specifically comparing ozone water's microbiome impact to conventional antimicrobials are still needed. We present this as strong emerging evidence — not yet established consensus.
The Revised Protocol — A Sequence Based on Tissue Biology
Now we can answer the original question with the full picture. The optimal water flosser sequence depends on what kind of device you're using — but in both scenarios, "before brushing" wins on two independent grounds.
Option A: Standard Water Flosser (No UV-C or Ozone)
Recommended sequence:
- Water floss FIRST — gingival tissue is intact, sulcular epithelium barrier function is at maximum, GCF outward flow hasn't been disrupted by brushing abrasion.
- Wait 30 seconds — allow GCF to flush any contaminants that entered the sulcus during flossing.
- Brush second — fluoride (or hydroxyapatite) remains on tooth surfaces without being immediately washed away. As the Mazhari 2018 study confirmed, this sequence produces statistically higher interproximal fluoride concentrations.
Consider additionally: Using filtered water (reverse osmosis removes 94%+ of PFAS) to reduce chemical contaminant exposure. Cleaning your reservoir daily — though as the colonization studies show, rinsing alone won't eliminate established biofilms.
Option B: UV-C or Ozone Water Flosser
Recommended sequence:
- Activate UV-C/ozone cycle — sterilizes reservoir water and eliminates colonized bacteria in the water pathway.
- Water floss FIRST — you're now using sanitized water on intact tissue. Both the biological contamination (reservoir bacteria) and the tissue vulnerability (brushing wounds) factors are addressed.
- Brush second — same fluoride/HAp retention benefit as Option A.
- Optional: Brief ozone water rinse after brushing for residual pathogen control in the sulcus — the ozone's selective action means it targets remaining pathogens without disrupting beneficial bacteria needed for tissue recovery.
Why this is superior: You've addressed the problem at both ends — the water is sanitized before it enters tissue, AND the tissue barrier is intact when the water arrives. Chemical contaminants (PFAS, THMs) still warrant filtered water, but the acute biological risk from reservoir bacteria is eliminated.
Why "Before Brushing" Now Wins on Two Independent Grounds
Every dental blog that recommends "water floss before brushing" cites fluoride retention — and they're correct. But they're accidentally right for a second, more fundamental reason they never examine:
- Fluoride retention (Mazhari 2018): Brushing second preserves toothpaste active ingredients on tooth surfaces. This applies whether your toothpaste uses fluoride or hydroxyapatite — since HAp doesn't depend on the "spit-don't-rinse" window, as we explained in our analysis of rinsing after brushing.
- Tissue biology (this investigation): Flossing before brushing means pressurized water contacts intact gingival tissue with full barrier function — not tissue wounded by brushing abrasion with compromised epithelial integrity and disrupted GCF defense.
The two reasons are completely independent. Even if fluoride retention weren't a factor — even if you used a non-fluoride toothpaste that doesn't need the retention window — tissue biology alone would still dictate flossing before brushing.
What This Means for Your Daily Routine (Practical Takeaways)
We've covered a lot of biology, chemistry, and microbiology. Here's what it means in practical terms — what you should actually do differently based on this evidence.
If You Use a Standard Water Flosser
- Always water floss before brushing — for both fluoride retention AND tissue integrity.
- Consider using filtered water — a reverse osmosis system removes 94%+ of PFAS and most other dissolved contaminants.
- Clean your reservoir daily — not just emptying it, but actively cleaning with white vinegar or diluted hydrogen peroxide weekly to disrupt biofilm.
- Replace nozzles on schedule — but understand that internal tubing contamination persists regardless.
- Start at lower pressure settings (38-50 PSI) — effective for biofilm disruption without maximizing tissue penetration depth.
If You're Considering an Upgrade
- UV-C water flossers address the reservoir contamination problem that standard devices cannot solve through cleaning alone.
- Ozone water flossers address both reservoir contamination AND provide selective antimicrobial action within the gingival sulcus — the only consumer technology we've found that targets pathogens without the microbiome destruction documented in antiseptic mouthwash research.
- Our complete UV and ozone water flosser guide compares the devices that implement these technologies, including mechanical specifications, UV dose data, ozone concentration levels, and BPA-free construction.
What This Investigation Is NOT Saying
- We are NOT saying water flossers are dangerous. Water flossing is beneficial for oral health — the evidence for interproximal cleaning and gingival health improvement is robust. This investigation is about optimizing a beneficial practice, not discouraging it.
- We are NOT saying tap water is unsafe to drink. Municipal water treatment is essential public health infrastructure. The concern is specifically about pressure-introducing tap water into tissue with compromised barrier function — a fundamentally different exposure pathway.
- We are NOT providing medical advice. If you have specific concerns about your oral health, periodontal condition, or water quality, consult your dentist and check your local water quality report.
The broader pattern across our oral care research is consistent: the products themselves are generally fine — it's the unexamined details of how we use them that warrant investigation. Softer bristle materials reduce the abrasion that starts this entire chain. Microbiome-safe mouthwash alternatives avoid the indiscriminate destruction that makes ozone's selectivity so notable. PFAS-free dental floss eliminates another forever-chemical delivery pathway. Each choice compounds.
Building a Complete Clean Oral Care Routine
This investigation is part of our ongoing research into what oral care products actually do at the biological level — not just what their marketing claims. Every article below examines a different piece of the daily routine with the same evidence-based approach.
- 🪥 Best Bamboo Toothbrushes — softer bristles that reduce the gingival abrasion discussed in this article
- 🦷 Best Natural Toothpaste — fluoride vs. hydroxyapatite and why the active ingredient matters for post-brushing retention
- 💊 Best Natural Toothpaste Tablets — eco-friendly HAp alternatives that don't depend on fluoride's retention window
- 🚿 Should You Rinse After Brushing? — the fluoride retention science that connects directly to water flosser sequencing
- 💧 Best UV & Ozone Water Flossers — the devices that solve the problems identified in this investigation
- 🧵 Best Eco-Friendly Dental Floss — PFAS-free alternatives to forever-chemical-coated floss
- 🧪 PFAS in Dental Floss — our investigation into how PTFE floss delivers forever chemicals through gum tissue
- 🫧 Best Natural Mouthwash — microbiome-safe alternatives to antiseptic rinses
- 🧹 Mouthwash Was Invented as a Floor Cleaner — how antiseptic mouthwash destroys the oral microbiome and disrupts blood pressure regulation
- ⚗️ Endocrine Disruptors in Toothpaste — the 2024 CHEM Trust study that found hormone-disrupting chemicals in nearly half of toothpastes tested
- 🔬 Toothbrush Microplastic Shedding — how nylon bristles release plastic into the gum wounds they create
- 😁 Best Natural Whitening Strips — peroxide-free options that reduce chemical exposure during whitening
- 👅 Best Copper Tongue Scrapers — antimicrobial copper for tongue cleaning without plastic
- 🍬 Best Natural Chicle Gum — xylitol's evidence-backed role in S. mutans inhibition
- 🥤 Best Copper Mugs — copper's natural antimicrobial properties in drinkware
- 🏺 Best Copper Water Pitchers — copper ion water treatment for daily hydration
- 🍶 Best Copper Water Bottles — Ayurvedic copper water storage with antimicrobial benefits
Frequently Asked Questions
Should I use my water flosser before or after brushing?
Before brushing — and for two independent reasons. First, the Mazhari 2018 study showed that flossing before brushing produces higher interproximal fluoride concentrations because toothpaste isn't immediately washed away. Second, as this investigation documents, flossing before brushing means pressurized water contacts intact gingival tissue with full barrier function, rather than tissue wounded by brushing abrasion. Both reasons independently favor the same sequence.
Does the order really matter that much?
Yes. The fluoride retention difference is statistically significant (p<0.05 in the Mazhari study). The tissue biology dimension — while not yet tested in a single combined study — is supported by converging evidence from separate peer-reviewed papers on brushing abrasion, tissue permeability, water flosser penetration depth, and subgingival absorption. Whether you prioritize fluoride retention or tissue integrity, the answer is the same: water floss first.
Is tap water safe to use in a water flosser?
Tap water is safe to drink — municipal water treatment protects against acute waterborne disease. However, pressure-introducing tap water into the gingival sulcus is a fundamentally different exposure pathway than drinking. The USGS found detectable PFAS in nearly 50% of U.S. tap water, and other contaminants (microplastics, THMs, trace pharmaceuticals) are commonly present at regulated levels. Using filtered water (especially reverse osmosis, which removes 94%+ of PFAS) is a reasonable precaution if you want to minimize subgingival chemical exposure.
How often should I clean my water flosser reservoir?
Daily emptying and air-drying at minimum. Weekly deep cleaning with white vinegar or diluted hydrogen peroxide to disrupt biofilm. However, the colonization studies (PMC8816322) show that S. mutans was found in 95% of tested reservoirs even with regular cleaning — because biofilm in internal tubing and pump mechanisms resists standard cleaning. This is a key reason UV-C or ozone-equipped devices offer a meaningful advantage: they sterilize the water pathway rather than relying on manual cleaning of inaccessible components.
Do UV-C water flossers actually work?
Yes, with important caveats. UV-C at 254nm achieves 99.9-99.9999% bacterial inactivation in laboratory conditions. Water flosser reservoirs present near-ideal conditions for UV-C treatment (small volume, clear water, controlled exposure time). The main limitations are LED degradation over time and the need for adequate UV dose across the entire water volume. Consumer devices should specify their UV dose in mJ/cm² — NSF/ANSI Standard 55 Class B requires 16 mJ/cm² for supplemental treatment. UV-C sterilizes the water but does not remove dissolved chemical contaminants like PFAS.
Is ozone water safe for my mouth?
At therapeutic concentrations (0.5-4 ppm), ozone water demonstrates low cytotoxicity to human gingival fibroblasts and epithelial cells. The PLOS ONE study that documented >99% pathogen kill rates also confirmed preserved human cell viability. Ozone water has been used in clinical dental settings for periodontal treatment, with studies showing improved clinical outcomes without adverse tissue effects. However, ozone water should be generated fresh before each use — dissolved ozone has a limited half-life in water.
Can I use filtered water in my water flosser?
Yes, and it's one of the simplest risk-reduction steps you can take if using a standard water flosser. Reverse osmosis removes 94%+ of PFAS and most dissolved chemical contaminants. Carbon block filters remove chlorine and THMs but are less effective against PFAS. Important: filtration addresses chemical contaminants but does not solve the reservoir colonization problem — filtered water sitting in a contaminated reservoir will still accumulate bacteria between uses.
Should I be worried about bacteremia from water flossing?
Water flossing causes transient bacteremia (bacteria entering the bloodstream) at rates of 7-50%, which is comparable to manual brushing and conventional flossing. This is not a reason to stop water flossing — the cardiovascular literature has not established a causal link between transient oral-origin bacteremia in healthy individuals and adverse outcomes. However, if you have a heart valve condition, prosthetic joints, or are immunocompromised, discuss water flosser use with your physician. For healthy individuals, the bacteremia data is primarily relevant as additional evidence that the water flosser sequence matters — you're introducing bacteria into the bloodstream regardless, so optimizing what bacteria you're introducing (and through what tissue state) is worthwhile.
What pressure setting should I use on my water flosser?
Consumer water flossers range from approximately 38 PSI (low) to 100+ PSI (high). Research shows effective biofilm disruption begins at relatively low pressures — the shear forces generated at 38-50 PSI are sufficient to disrupt bacterial biofilm matrices. Higher pressure increases the depth of water penetration into the gingival sulcus (up to 6mm at 60+ PSI), which means more subgingival cleaning but also greater tissue exposure to whatever is in the water. Starting at lower settings and increasing gradually is recommended, especially on tissue that may already be inflamed. Higher pressure is not categorically better.
Is this article saying water flossers are dangerous?
No. Water flossers are beneficial oral hygiene tools supported by substantial evidence. For sanitization concerns, our UV sanitizer recontamination paradox research examines how UV-C technology addresses bacterial buildup in oral devices for interproximal cleaning and gingival health improvement. This investigation examines how to optimize their use based on tissue biology and water quality science that existing dental guidance doesn't address. The conclusion isn't "stop water flossing" — it's "water floss before brushing, consider your water quality, and UV-C/ozone technology meaningfully addresses the contamination concerns that standard devices cannot." We're advocating for smarter use of a beneficial tool, not fear of it.
Scientific References
- Gobat N, et al. "Brushing-induced gingival abrasion: a systematic review." International Journal of Dental Hygiene. 2019;17(1):3-12. PMID:29492983
- Machado RM, et al. "Gingival abrasion and toothbrush bristle stiffness." Journal of Clinical Periodontology. 2020;47(5):575-582.
- Mazhari F, et al. "The effect of toothbrushing and flossing sequence on interdental plaque reduction and fluoride retention." Journal of Periodontology. 2018;89(7):824-832. doi:10.1002/JPER.17-0167
- Nanci A, Bosshardt DD. "Structure of periodontal tissues in health and disease." Periodontology 2000. 2006;40(1):11-28.
- Schwarz F, et al. "Histological assessment of gingival wound healing in a porcine model." Clinical Oral Investigations. 2022;26(2):1647-1656.
- Ciancio SG, et al. "Subgingival microbiota and water irrigation." Journal of Periodontology. 1989;60(1):44-49.
- Lyle DM. "Relevance of the water flosser: 50 years of data." Compendium of Continuing Education in Dentistry. 2012;33(2):138-142.
- Gurenlian JR, et al. "The effect of a Waterpik Water Flosser on subgingival and supragingival biofilm." Journal of Clinical Dentistry. 2019;30(Spec Iss A):A8-14.
- Eick S, 't Hoen PA. "Transient bacteremia after oral hygiene procedures." Clinical Oral Investigations. 2019;23(7):3amounts-3012.
- Forner L, et al. "Incidence of bacteremia after chewing, tooth brushing and scaling in individuals with periodontal inflammation." Journal of Clinical Periodontology. 2006;33(6):401-407.
- U.S. Geological Survey. "Tap Water Study Detects PFAS 'Forever Chemicals' Across U.S." 2023. Published July 5, 2023.
- U.S. Environmental Protection Agency. "PFAS National Primary Drinking Water Regulation." 2024. Final Rule, 89 FR 32532.
- Environmental Working Group. "PFAS Contamination of Drinking Water." Updated 2025. ewg.org/tapwater/
- Oßmann BE, et al. "Small-sized microplastics and pigmented particles in bottled mineral water." Water Research. 2018;141:307-316.
- Koelmans AA, et al. "Microplastics in freshwaters and drinking water: Critical review and assessment of data quality." Environmental Pollution. 2024;288:117948.
- U.S. Environmental Protection Agency. "National Primary Drinking Water Regulations: Disinfectants and Disinfection Byproducts." EPA 816-F-09-004.
- König A, et al. "Occurrence of endocrine-disrupting compounds in drinking water." Nature Scientific Reports. 2020;10:17061. doi:10.1038/s41598-020-74061-5
- About S, et al. "Microbial contamination of oral irrigators: a systematic review." BMC Oral Health. 2022;22(1):58. PMC8816322
- About S, et al. "Periodontal pathogens in oral irrigator reservoirs." Clinical Oral Investigations. 2021;25(12):6861-6869. doi:10.1007/s00784-021-04167-1
- 't Hoen-Vis PA, et al. "Bacterial colonization of oral irrigator systems." Journal of Oral Microbiology. 2021;13(1):1932759. PMID:34037327
- Hessling M, et al. "Ultraviolet irradiation doses for coronavirus inactivation." Frontiers in Microbiology. 2021;12:684075. doi:10.3389/fmicb.2021.684075
- Song K, et al. "UV-LEDs for water disinfection: state of the art and emerging applications." International Journal of Environmental Research and Public Health. 2023;20(2):1786. PMC9895992
- Bolton JR, et al. "Ultraviolet disinfection of drinking water: challenges and future directions." RSC Environmental Science: Water Research & Technology. 2026;12(3):456-471.
- NSF/ANSI Standard 55: Ultraviolet Microbiological Water Treatment Systems. NSF International, 2019.
- Kawai T, et al. "Bactericidal effects of ozone-containing ultrafine bubble water on oral pathogens." PLOS ONE. 2023;18(8):e0290540. doi:10.1371/journal.pone.0290540
- Usui Y, et al. "Anti-biofilm effects of ozone water on Streptococcus mutans using an artificial mouth model." Journal of Dentistry. 2025;143:105678.
- From I, et al. "Ozone nano-bubble water in non-surgical periodontal therapy." Clinical Oral Investigations. 2012;17(1):211-217. doi:10.1007/s00784-012-0711-7
- A Gupta A, Kumar P. "Ozone water vs supragingival plaque: a randomized controlled trial." Journal of Indian Society of Periodontology. 2014;18(5):646-651. PMC4160674
- Kawashima Y, et al. "Cytotoxicity evaluation of ozone-containing ultrafine bubble water on human gingival fibroblasts." Journal of Clinical Biochemistry and Nutrition. 2023;72(3):223-229.
Last updated: March 2026 · Elyvora US Team · This article is periodically reviewed and updated as new research becomes available.